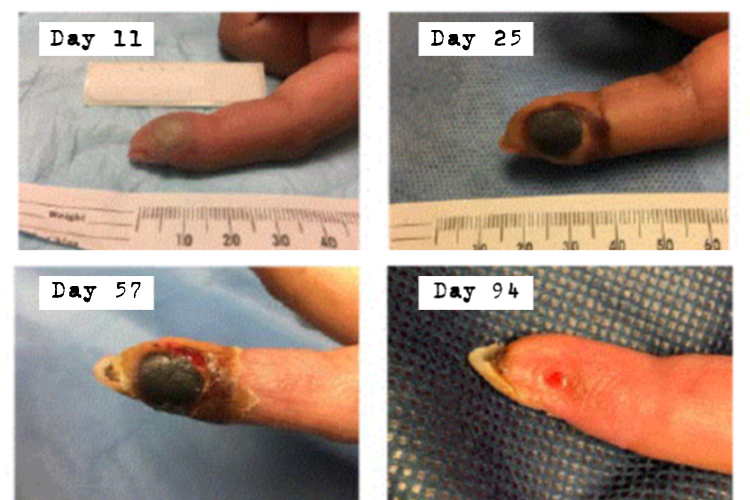
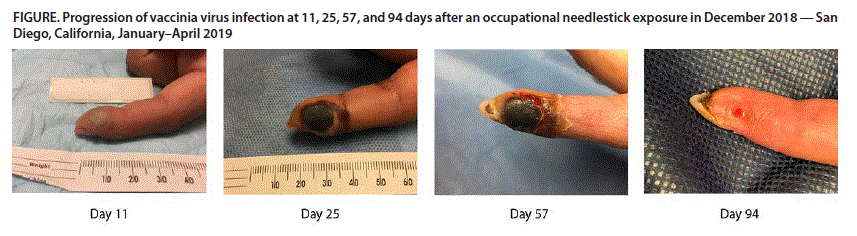
In December 2018, a lab technician was injecting a mouse with the Vaccinia Virus (VACV) when she accidentally stuck her own finger with the needle. According to the CDC’s case report, she immediately rinsed her finger with water for 15 minutes, notified her supervisors, then went to the emergency room.
Between days 2 and 9 post-infection, the patient was evaluated by two community physicians; neither advised her to observe contact precautions to prevent auto-inoculation or secondary transmission. (source)
It should probably be pointed out that this happened almost a year ago and yet this was just published by the CDC on October 25, 2019, in the CDC’s Morbidity and Mortality Weekly Report (MMWR).
Secondly, the Vaccinia Virus is contagious – it can be spread through physical contact, and yet the technician was not told to observe “contact precautions”, at least by the community physicians. While it is known that the tech’s recovery took approximately 4 months, the focus of the published report (as indicated in the title itself) was of the “novel treatment” that was performed. Folks, these facts ought to make you a bit nervous.
Ten days after the infection the technician was evaluated at an occupational health clinic where the treating physician contacted the CDC, which advised monitoring her for evidence of worsening infection.
(image source: CDC)
Twelve days post-infection she was treated at a university-based ER for a fever, a general feeling of illness, pain, and worsening swelling of her finger. This means she was seen at two different facilities, and by at least three different doctors, possibly without taking precautions to prevent others from getting infected. I say ‘possibly’ because while she wasn’t told to by supervisors, she may have taken precautions on her own. We can only hope.
Subscribe to our newsletter
Trying to figure out how to stock up while prices keep climbing? We can help with our free guide and newsletter!
The threat of Poxviruses
Contagious, often deadly, and naturally occurring (meaning it exists in nature), smallpox was considered eradicated around the globe by 1980. With the exception, of course, of the two labs that currently hold samples of the smallpox virus for research – although the one in Russia did have an explosion in September of this year. That being said, I sometimes wonder how long it will be before tight-lipped Russian authorities speak up if any smallpox was leaked out… But that’s just my opinion.
According to the National Library of Medicine at the National Institutes of Health, smallpox is caused by an agent referred to as the variola virus, also known as VARV, and strictly affects humans. Most researchers agree that the first reliable descriptions of smallpox were found in ancient Indian medical treatises that had been compiled by the 1st–4th centuries. It wasn’t until 1796 that a vaccine was created by a man named Edward Jenner who had observed that milkmaids who previously had caught cowpox did not catch smallpox. While it’s not the exact same vaccine we have today, according to the World Health Organization there is a physical stockpile of smallpox vaccines held at various locations around the world – just in case.
At this point, I have to say ‘Hold on – not so fast there’. Smallpox is but one virus from the Pox family, known as Poxviruses (members of the Poxviridae family). Smallpox may be eradicated, but what about the others? Let me say, for clarity if nothing else, I’m not an epidemiologist. I have never done laboratory research on anything more than the odd creature in high school biology. But what I’ve read makes me nervous.
VACV is supposedly a very mild poxvirus and is used today as a live vaccine for other poxviruses like smallpox, and for experimental testing for cancer cures.
As pointed out earlier, Vaccinia is used for vaccines and vaccinations and is also Poxvirus. And there are a lot of poxviruses; just go here and click on any of the little + beside each one to see the genus. If you click on Orthopoxviruses, you’ll see both the Variola Virus (Smallpox) and the Vaccinia Virus (Smallpox Vaccine).
The Monkeypox virus
Included in the poxviruses is Monkeypox. The monkeypox virus is rare but belongs in the same genus as both vaccinia and smallpox. Despite the rarity, in 2003 there was an outbreak of monkeypox in the United States, and it was the first time human monkeypox was reported outside of Africa.
It was determined that a shipment of animals from Ghana imported to Texas on April 9, 2003, introduced the monkeypox virus to the US and there were 37 confirmed cases, with 18 of them in Wisconsin. It was transmitted to humans via infected prairie dogs purchased as pets. In this outbreak, the CDC, USDA, FDA, and other agencies assisted in containing the outbreak and many were advised to get the smallpox vaccination. For those infected, however, there is currently no proven safe treatment for the monkeypox virus infection. (If you recall, a virus usually must run its course – antibiotics only work on bacterial infections.) For purposes of controlling it, however, antivirals can be used.
The Brazilian Journal of Infectious Diseases, in April of 2010, stated that Brazil had experienced numerous outbreaks related to the vaccinia virus since 1960 by several research groups in differing regions:
Episodes of Vaccinia virus infection in people who work at research laboratories have already been reported by the Center for Disease Control and Prevention (CDC), contributing to increase the number of infection cases. The virus infection has occurred both in individuals previously vaccinated in childhood, and in people never vaccinated before. Transmission usually occurs through accidental inoculation of vaccinia virus through lesions in fingers and eyes, or through auto-inoculation. (source)
The journal entry goes on to say that in addition to laboratory infection, cases of person-to-person contamination have also been reported. Those cases are closely related to the vaccination of militaries against the smallpox virus. Some of those cases of infection were possibly transmitted through sexual contact between military members and non-military members. One case was reported in a pregnant woman that was bitten by a dog previously vaccinated against rabies, and many vaccinia virus infections in Brazil can be characterized as zoonotic infections as they occur in human beings who work directly with cattle.
What are the signs and symptoms of Poxvirus infection?
The symptoms can vary depending on the genus, but the CDC lists the following:
- Fever
- Headache
- Muscle aches
- Backache
- Swollen Lymph nodes
- Chills
- Exhaustion
Within 1-3 days a rash usually appears, and the whole infection can last a month easily. Thankfully there are ways we can help prevent a poxvirus infection.
- Avoid contact with animals that could have the virus or are sick.
- Avoid contact with any bedding or other such materials that have been in contact with a sick animal.
- Isolate infected patients from others who could be at risk for infection.
- Wash your hands and arms thoroughly with soap after contact with infected animals or humans, and consider using an alcohol-based hand sanitizer. (Remember that any hand sanitizer does not take the place of good old soap and water.)
- Try to use personal protective equipment in the form of masks, gloves, and overclothes when caring for someone who is infected.
Are you prepared for an outbreak?
In the future, we may never have to worry about poxviruses. I, for one, hope that’s the case, but it’s certainly worth it to be prepared in case we do.
It frightens me how much goes on in laboratories and research facilities that we simply don’t know about, and while doing research for this article I realized just how much I don’t know about the world of viruses; and just how easily one can cross over to us humans.
For more information on viruses, bacteria, and even preparing for a possible pandemic, I recommend reading the following:
- Prepping For A Pandemic by Cat Ellis
- Are You Prepped For A Pandemic? by Daisy Luther
- There Seems To Be Growing Concern About Biological Attacks by Daisy Luther
What are your thoughts on this?
Would you rather know at the time or after the fact? How much do you think is being hidden from us about this type of research? Share what you think in the comments.
About Sandra
Sandra is a published artist, photographer, fellow prepper, and animal advocate.














12 Responses
Yes I’d prefer knowing sooner than later. But not being told sounds par for government secrecy.
Just recently read an article that reported the CDC is a private, for-profit entity.
They are financed by Big Pharma and other large “medical” corporations, particularly ones that produce (hold on to your hat) vaccines.
Huh.
It’s probably no surprise to folks here, but the gen pop just doesn’t seem to understand that the CDC is not looking out for the health of the people, but rather for the health of their corporate sponsors’ bottom line.
CDC is a private, for profit entity, owned by big pharma, huh? It figures. When in doubt, follow the money.
The CDC (Centers for Disease Control) is NOT a private organization. It is a federal agency. Wikipedia’s article about the CDC seems to be fairly accurate — https://en.wikipedia.org/wiki/Centers_for_Disease_Control_and_Prevention
You can also go directly to the CDC web site at https://www.cdc.gov/
The CDC Foundation IS a nonprofit organization established by Congree in order to allow philanthropic organizations, businesses, etc. to collaborate with the CDC. That may be where the confusion comes in–especially if there is a possible conflict of interest, and, at times, that could be the case. The claim is that there are review procedures in place to “safeguard against possible conflicts of interest.” See info about the Foundation here: https://www.cdcfoundation.org/FAQ
The CDC has a huge budget and employs more than 15,000 people. The agency does a lot of things. One little-known thing it does is run the NPCR (National Program of Cancer Registries) which funds and guides the state cancer registries. De-identified information about cancer cases (de-identified meaning no personal information about the patient is given) is sent from hospitals, oncology clinics, etc. to the state registries who then perform all sorts of data analysis about what treatments are occurring in an area and what treatments are working against those cancers. This is the type of data that is used to create guidelines for cancer treatment that are “evidence-based.” If you ever have cancer, you want your oncologist to have access to this type of information. (Yes, I know I will get responses about just eating natural foods, etc., for cancer, but I have had two relatives who had the cleanest, most-natural diets in the world and they both died of cancer–one at a young age. There may be problems with the CDC working with private organizations, but I know they also do a lot of good work in other areas.
Cheryl,YOUR hero’s at the CDC are all demons from HELL,and thats where their going when they leave this world,cancer cures have been HIDDEN BY THE CDC for at least 50 years by the CDC,cancer will never be cured in america as long as the CDC exists and the BIO-WARFARE CENTER at FT.DETRICK MARYLAND,their the ones who created every cancer you ever heard of,THESE FILTH ARE NOT HERO’S….
Wow! I didn’t know the CDC existed in 3000 B.C.! That is when the earliest cases were first mentioned. (There is a brief history written in an easy-to-read format:
https://www.canaryfoundation.org/2012/08/13/how-long-have-we-been-plagued-by-cancer/
(BTW, I don’t know anything about the Canary Foundation, I was just looking for an interesting easy-to-read article. I have not researched them and know nothing about them. Of course, some of you don’t have to research anything. You have an automatic opinion. ANYBODY doing ANYTHING is part of some deep, dark government conspiracy to ruin EVERYONE’s life in America… or maybe the world. Yes, I think it’s the WORLD!!!!)
Seriously, I do know there is an advertisement/email on the web about how the government has concealed the cure to cancer, and if you get this person’s herbs/vitamins, or whatever, you can beat cancer. As far as I know, that is the only “source” I have seen about this conspiracy theory. This reads more like an advertisement to sell a product to me.
I have no problem believing that our government is less than honest in many areas. However, I would prefer to have some sources mentioned with some actual data that supports this. Anyone that has some concrete evidence, I would be happy to examine it. Truly, nothing would make me happier than to find that INDEED the government has suppressed the cure for cancer and we just need to do A, B, C to stop the disease.
I feel that the public should have been informed. As well as the doctors who treated the infected patient. I had the small pox vaccine when I was in grade school. Many years ago. Our health is very important. We need to be informed of any and all diseases that are contagious.
Damn! That’s frightening…a) that the CDC doesn’t release this sort of information, b) that the information woman was not quarantined and doctors didn’t seem to take better precautions, and c) it seems that the CDC was poised for a cover up in case the virus became widespread. As it turned out, apparently the technician was the only one who got sick… could have been so much worse.
As I’ve said before, the CDC labs should not be in a heavily populated area for this reason.
Seeing that the CDC was injecting a mouse with the virus then possible they made the virus like many other viruses. The Bible tell us in the end times ( which we are in) there will be diseases and pestilences. There are so many strange named viruses. If they create the virus then they can create a vaccine for it or maybe to thin the population as some are saying. We all need to trust in God!!!!!
I received this wierd error message when trying to post my response:
Error Code 5541
This request has been blocked by WebARX Web Application Firewall .
If you are a legitimate user, contact the administrator of the site with above error code if this message persists.
Return To Homepage
So, the ‘cliff notes’ version of my original reply (do cliff notes still exist LOL?)
There were many mis-steps in the handling of this situation, based on my medical background, which does not include epidemiology/research. This person should never have gone to a ‘public’ medical facility, unless the research facility had a contract with them, which should have raised alerts immediately.
The fact of the matter is, these things are happening all around us, every day. We only get alerted when it fits ‘the agenda’. Which is why we stay alert and prepared.
Is the CDC really an organization focussed / concerned with health issues ? . . . Efforts were made to report a mail order can of cashews that smelled and tasted tainted with a petroleum product . . . And, the reaction / response ? . . . N O N E . . . N A D A . . . N O T H I NG